AI-Powered
Dental RCM
Spend time with patients,
not portals
Dental Insurance Collections Per Year
$26M


Powered by AI. Verified by dental billing experts with
10+

Years of Experience
Net Collections
98%
95% First Pass Clean Claims Rate

What Success Looks Like
What we offer
End to End RCM
Service
From patient intake to final payment, our comprehensive revenue cycle management handles every step. Reduce claim denials, accelerate reimbursements, and maximize collections with intelligent automation that keeps your revenue flowing.
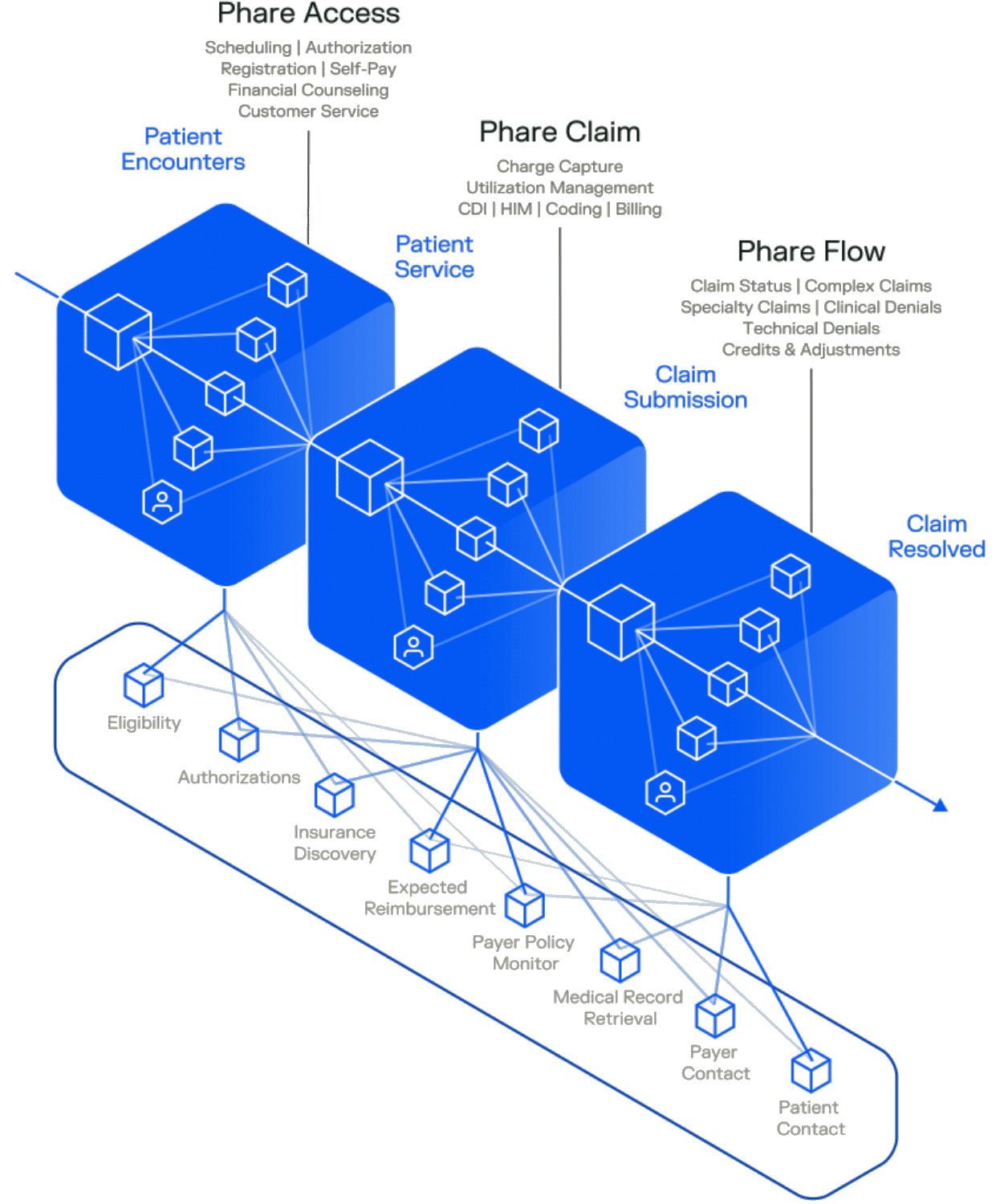

Chatgpt for your practice
AI Financial Advisor
Get personalized financial guidance powered by advanced AI that analyzes your complete financial picture. From investment strategies to cash flow optimization, make smarter decisions with insights tailored to your goals.

Primerose Dental achieved 40% reduction in coding denials
We take Medicaid, CHIP, all of it. And the coding rules are brutal. One wrong modifier and you're denied. We were losing money and patients' trust just trying to keep up. Since switching to Lavender, coding denials dropped 40%. My front desk finally has time to actually talk to patients.
Dr. Nishi Arondekar
Owner

We work with ALL EHRs


And more...
Our team
Thanks to our clients, friends, partners and to our whole team who made this journey possible.
.webp)



.webp)
.png)
.jpeg)
FAQs
Everything you need to know about the product and billing. Can’t find the answer you’re looking for? Please chat to our team.
How does AI actually improve my collections compared to a regular billing company?
Our AI catches errors humans miss. It analyzes patterns across millions of claims to predict which codes will be denied by specific insurance carriers before submission. It cross-references patient history, insurance rules, and payer-specific requirements in seconds. Result: 97% first-pass acceptance rate vs industry average of 85%, meaning you get paid 2-3 weeks faster and avoid the denial/resubmission cycle that loses money.
How does your AI handle insurance verification differently?
Traditional verification is a phone call where staff check basic eligibility. Our AI digs deeper in real-time: it verifies eligibility, checks remaining benefits, identifies frequency limitations, flags pre-auth requirements, detects dual coverage scenarios, and analyzes historical claim data from that specific payer to predict potential issues. You get a complete financial picture 48 hours before the patient arrives, not a basic "yes they have coverage" check
How long does implementation take and will I lose claims during transition?
7-10 days for full setup. We run parallel with your current system initially so zero claims are lost. Our team handles all technical integration with your EHR. Your front desk training takes about 2 hours. Most practices are fully transitioned within 2 weeks with no revenue disruption.
What if I already have a billing team in-house?
Many practices transition their billing staff to patient coordination and treatment planning - higher value work. Some keep one biller for oversight while we handle the volume. Either way, you'll reduce overhead while collecting more. We can show you the math on your current vs projected costs during a consultation.
What proof do you have that this actually works?
Our case studies show practices going from 86% to 98% collections within 90 days. We've collected over $60M in dental insurance. You can talk directly to our current clients during your trial period.



